AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Meld score 191/14/2024 
Measurement of the severity of portal hypertension via the HVPG is an intuitive first step in identifying at-risk patients based on physiology. 14 Most center around quantification of portal hypertension and its sequelae. Many potential candidates for predictors have been suggested and examined in the past. The remainder of this paper describes potential candidates for these attributes Future work should concentrate on identifying high risk attributes of patients within this low MELD-Na cohort to help determine subgroups that would benefit from earlier transplant. Despite these changes, it remains unclear how to identify which low MELD-Na patients will continue to suffer from liver related morbidity and mortality.Īs scoring systems are improved, the patients with consistently low scores are distilled into a truly low risk group. 10, 13 Ultimately, the MELD-Sodium (MELD-Na) score was officially incorporated into organ allocation in 2016. Furthermore, this effect is present even up until a MELD score of 38. 10 In fact, in patients with a MELD score less than 21, only serum sodium and persistent ascites, but not MELD, were significantly associated with waitlist mortality. 10, 12 This is particularly true of patients with low MELD scores, where the effect of serum sodium is significantly greater. 9– 12 In particular, hyponatremia has been established as a key predictor of mortality. 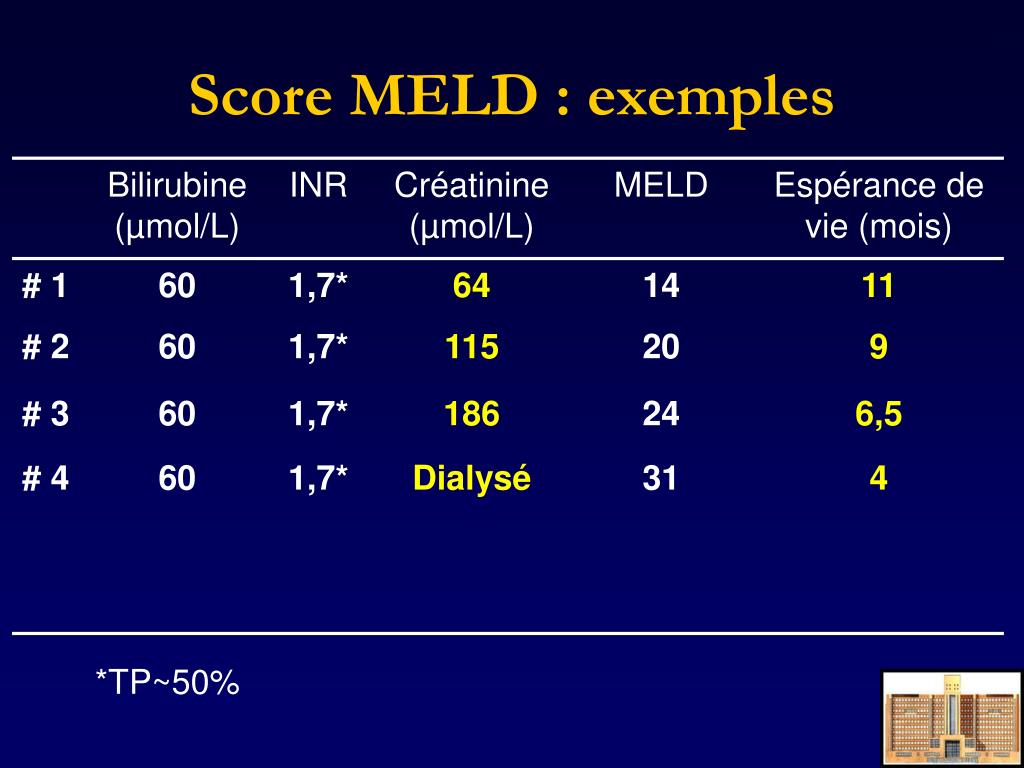
In fact, at lower scores MELD’s prognostic capability has been noted to be inferior to serum sodium, ascites, encephalopathy, glomerular filtration rate (GFR), and CTP score. 1, 8 This model for end-stage liver disease (‘MELD score’), based on bilirubin, creatinine, and INR, was adopted for organ allocation in the United States in 2002.Ĭriticism of the MELD score stems from the basis of its conception as a risk prediction model for patients with Child C cirrhosis and its focus on short term, 90 day mortality. A logistic regression model for predicting 3-month mortality was noted to be superior to the CTP score in this group undergoing elective TIPS with further analysis validating its prognostic capability for decompensated liver cirrhosis and prediction of waitlist mortality. 7 With the rise of interventional radiology and placement of transjugular intrahepatic portosystemic shunts (TIPS) there was again an increase in mortality in the sub-population of patients with CTP class C cirrhosis. 6 In 1973, Pugh et al provided a revised score which substituted prothrombin time in place of nutritional status to form the Child-Turcotte-Pugh (CTP) score. In the early 1950s, Child and Turcotte attempted to identify high risk patients by laboratory factors (serum bilirubin and albumin) and clinical factors (ascites, encephalopathy, nutritional status) prior to surgery for portal hypertension. 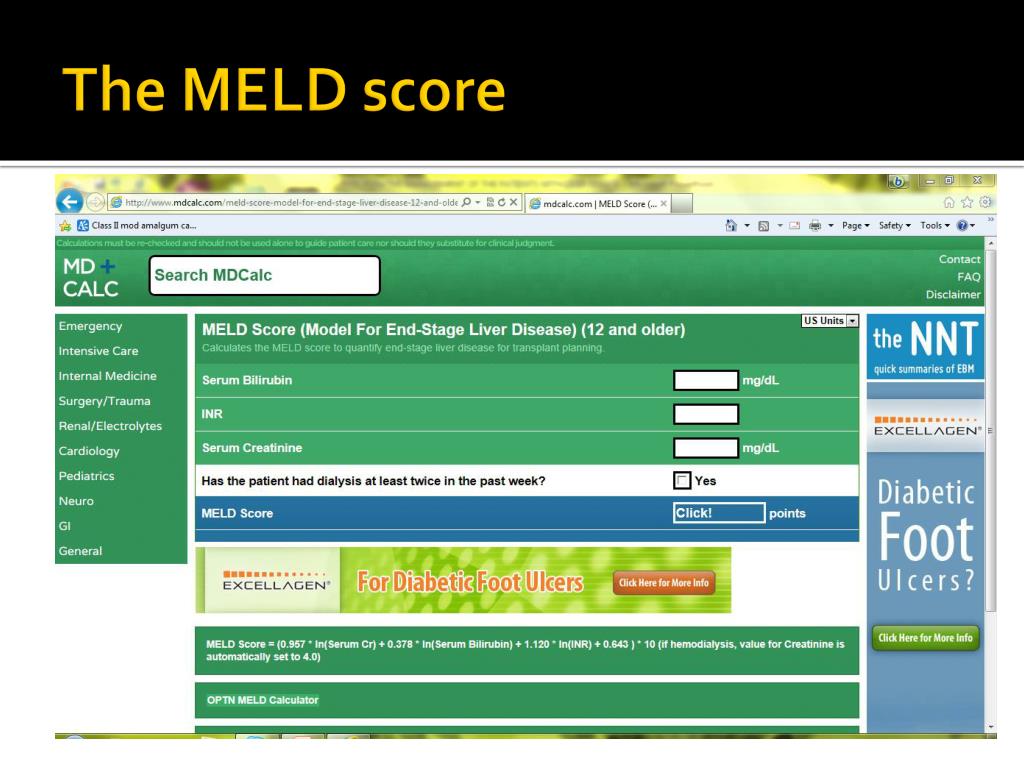
4, 5 Although most research has been done prior to the MELD-Na score, we review the literature on historical and novel factors that might be extended to identify the group of ‘low MELD-Na’ patients who suffer liver related complications and may benefit from earlier liver transplant, the use of more marginal liver grafts, or more intensive nontransplant treatments.Ī Brief History of Risk Scoring for Liver Disease SeverityĪdvancements in risk prediction for liver disease severity have been largely driven by identifying populations at high risk for complications after procedures. 3 Furthermore, the vast majority of patients listed for transplant must deal with this issue, with a 2004 study finding 92% of waitlisted patients had a MELD score of 18 or less and a more recent 2014 analysis noting 73.4% of patients were initially listed with a MELD less than 16. 1, 2 However, though patients with lower MELD-Na scores are de-prioritized with regards to liver transplant, they may still have a significant burden of liver related mortality. The Model for End Stage Liver Disease – Sodium (MELD-Na) score has been repeatedly shown to accurately predict three month mortality at high scores and is currently used to prioritize recipients for liver transplant allocation. Nowhere has this been more apparent than in the field of end stage liver disease and liver transplantation where sparse organ availability has required careful allocation. With increasingly modern approaches, patients can be prioritized for life saving procedures or maneuvered away from potentially dangerous ones. Prediction and prognosis has been a quintessential aspect of the art of medicine since its inception.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
